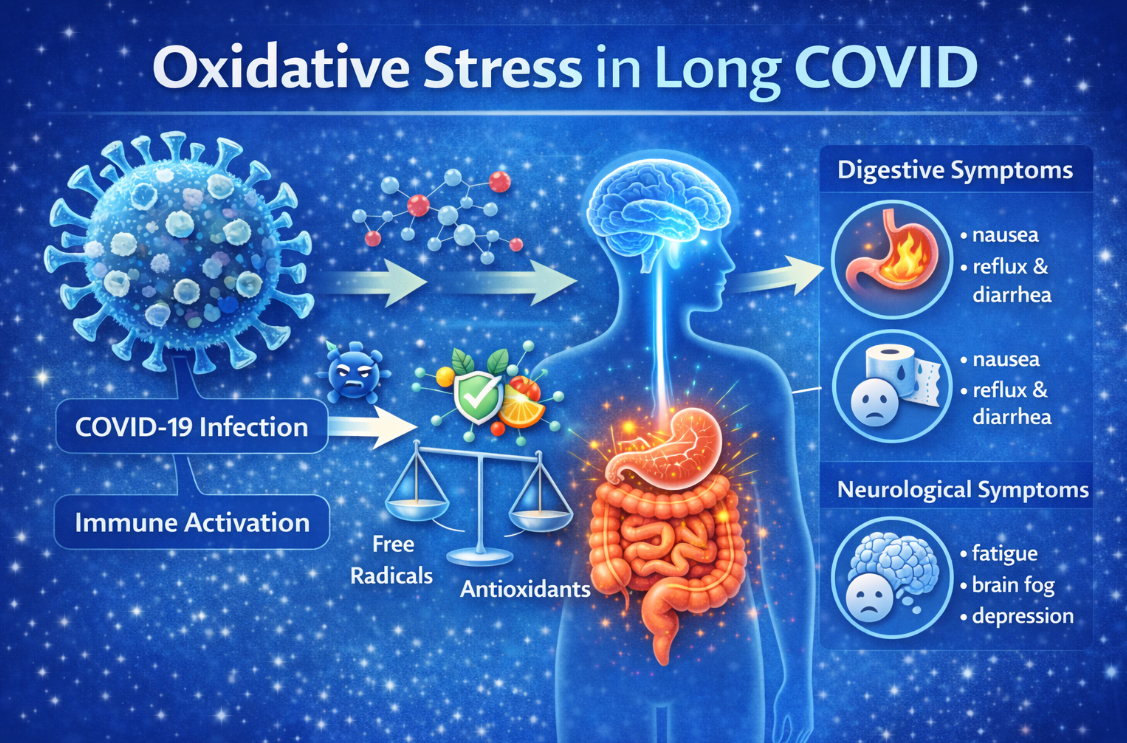
Long COVID and Oxidative Stress: Brain Fog, Fatigue, and Cellular Damage Explained
Long COVID and Oxidative Stress: Is Your Brain “Rusting”?
What if your brain isn’t tired because you’re busy, but because it’s under constant microscopic stress? Stay with us.
Most people blame fatigue and brain fog on stress, poor sleep, aging, or burnout.
But there’s a quieter, often overlooked driver behind many Long COVID symptoms:
👉 Oxidative stress
What is Oxidative Stress? (Simple Explanation)
Oxidative stress occurs when there is an imbalance between:
Free radicals (unstable molecules that damage cells)
ANDAntioxidants (your body’s defense system)
Think of it like this:
Oxidative stress = internal “rusting” of your cells
When this process goes unchecked, it can damage:
brain cells
mitochondria (your energy production centers)
blood vessels
immune function
Why This Matters in Long COVID
Emerging research suggests that oxidative stress plays a central role in Long COVID (PASC).
After a COVID-19 infection, the body may remain in a state of:
chronic inflammation
immune activation
mitochondrial dysfunction
This creates the perfect environment for oxidative stress to persist.
Common Long COVID symptoms linked to oxidative stress:
brain fog
fatigue
headaches
dizziness
exercise intolerance
mood changes
memory issues
In many cases, patients describe feeling like:
“I’m doing everything right… but something still feels off.”
This may be why.
The Brain Is One of the First Affected Systems
The brain is especially vulnerable to oxidative stress because it:
uses a large amount of oxygen
has high metabolic demand
relies heavily on mitochondrial function
When oxidative stress increases, it can disrupt:
neurotransmitter (hormone) balance
blood flow
energy production
This contributes directly to:
cognitive dysfunction
slowed processing
sensory sensitivity
sleep disturbances
Glutathione: Your Body’s Master Antioxidant
One of the most important defenses against oxidative stress is:
👉 Glutathione
Glutathione helps:
neutralize free radicals
detoxify harmful substances
support immune regulation
protect brain and mitochondrial function
Key insights:
Levels naturally decline with age (often starting in your 30s)
Illness, stress, and inflammation accelerate depletion
COVID-19 may significantly reduce glutathione availability
This has led researchers to explore glutathione depletion as a key factor in Long COVID symptom persistence.
Why Many People Don’t Improve (Even When “Doing Everything Right”)
One of the challenges with oxidative stress is that:
👉 It happens at the cellular level
Even if someone is:
eating well
exercising (within tolerance)
sleeping better
taking supplements
They may still struggle if:
nutrients are not reaching the cells
inflammation remains elevated
mitochondrial dysfunction persists
This is why Long COVID recovery often requires a multi-system approach, not just symptom-based treatment.
Quick Recovery Strategies You Can Start Today
🧠 Quick Guide: How to Support Glutathione Levels in Long COVID
Supporting glutathione may help reduce oxidative stress and support energy, brain function, and recovery.
🥦 1. Focus on Glutathione-Building Foods
- Garlic and onions
- Cruciferous vegetables (broccoli, kale, Brussels sprouts)
- Lean protein (chicken, fish, eggs)
- Legumes and nuts
🍓 2. Increase Antioxidant Intake
- Berries (blueberries, strawberries)
- Leafy greens (spinach, arugula)
- Citrus fruits (oranges, lemons)
- Colorful vegetables (peppers, carrots)
💊 3. Consider Targeted Supplements (with provider guidance)
- N-acetylcysteine (NAC)
- Alpha-lipoic acid (ALA)
- Liposomal glutathione
- Vitamin C (supports recycling of glutathione)
🚶♀️ 4. Support Your System with Gentle Movement
- Walking
- Stretching or yoga
- Breathwork
⚠️ Avoid overexertion — pushing too hard can increase oxidative stress in Long COVID.
😌 5. Regulate the Nervous System
- Prioritize sleep
- Reduce stress triggers
- Use pacing strategies
- Limit overstimulation when symptomatic
💡 Pro Tip
If you feel like you’re “doing everything right” but still struggling, oxidative stress at the cellular level may be a missing piece.
⚕️ Important
Always discuss supplements and treatment strategies with a qualified healthcare provider—especially in complex conditions like Long COVID.
💬 Why this matters
Addressing oxidative stress is not just about energy—it may help support:
- brain fog
- fatigue
- inflammation
- overall system stability
What Contributes to Ongoing Oxidative Stress?
In Long COVID, oxidative stress may be driven by:
persistent immune activation
mitochondrial dysfunction
mast cell activation (MCAS)
chronic inflammation
autonomic nervous system dysregulation
psychological stress (PTSD, illness trauma)
Even everyday factors can worsen the burden:
travel
overexertion
poor sleep
emotional stress
Supporting the Body Against Oxidative Stress
While research is ongoing, strategies that may help reduce oxidative stress include:
Foundational Support
Anti-inflammatory nutrition
Adequate hydration
Sleep optimization
Stress reduction
Nervous System Regulation
Breathwork
Pacing strategies
Reducing overstimulation
Nutritional & Clinical Considerations
Antioxidant support (as clinically appropriate)
Mitochondrial support
Addressing histamine and MCAS if present
⚠️ Always consult with a qualified provider before starting new treatments or supplements.
Supporting Glutathione Levels
Supporting glutathione production is a key strategy in reducing oxidative stress, particularly in Long COVID where depletion may occur due to ongoing inflammation. The body produces glutathione from amino acids, so nutrition plays a foundational role. Foods rich in sulfur-containing compounds—such as garlic, onions, cruciferous vegetables (broccoli, Brussels sprouts, kale), and high-quality protein sources—help provide the building blocks needed for synthesis. Antioxidant-rich foods like berries, leafy greens, and citrus fruits may also support overall redox balance.
From a supplementation perspective, compounds such as N-acetylcysteine (NAC), alpha-lipoic acid, and liposomal glutathione are often used clinically to help replenish intracellular levels, though absorption and individual response can vary. Regular, gentle physical activity within tolerance such as walking, stretching, or breathwork may also support endogenous antioxidant systems and mitochondrial function. However, overexertion can increase oxidative stress in Long COVID patients, so pacing is critical.
As always, interventions should be individualized and discussed with a qualified healthcare provider, particularly in complex post-viral conditions.
Why This Matters for Recovery
Understanding oxidative stress helps shift the narrative from:
❌ “Why am I not getting better?”
➡️
✅ “What is happening at the cellular level that needs support?”
Long COVID is not simply fatigue or deconditioning—it is often a complex, multi-system physiological response.
And oxidative stress may be one of the key drivers behind it.
What support options exist for Long COVID patients?
Many individuals benefit from structured support navigating care, pacing, and recovery planning.
ProMedView offers:
✔ Chronic Illness Coaching & Advocacy
✔ Long COVID Recovery Coaching
These services focus on helping individuals regain stability, communicate with providers, and plan recovery.
References
Delgado-Roche L, Mesta F.
Oxidative Stress as Key Player in Severe Acute Respiratory Syndrome Coronavirus (SARS-CoV) Infection.
Arch Med Res. 2020.
Cecchini R, Cecchini AL.
SARS-CoV-2 infection pathogenesis is related to oxidative stress as a response to aggression.
Med Hypotheses. 2020.
Polonikov A.
Endogenous Deficiency of Glutathione as the Most Likely Cause of Serious Manifestations and Death in COVID-19 Patients.
ACS Infect Dis. 2020.
Nalbandian A et al.
Post-acute COVID-19 syndrome.
Nature Medicine. 2021.
Keywords:
Long COVID oxidative stress, brain fog COVID, glutathione Long COVID, fatigue PASC, mitochondrial dysfunction COVID, inflammation Long COVID