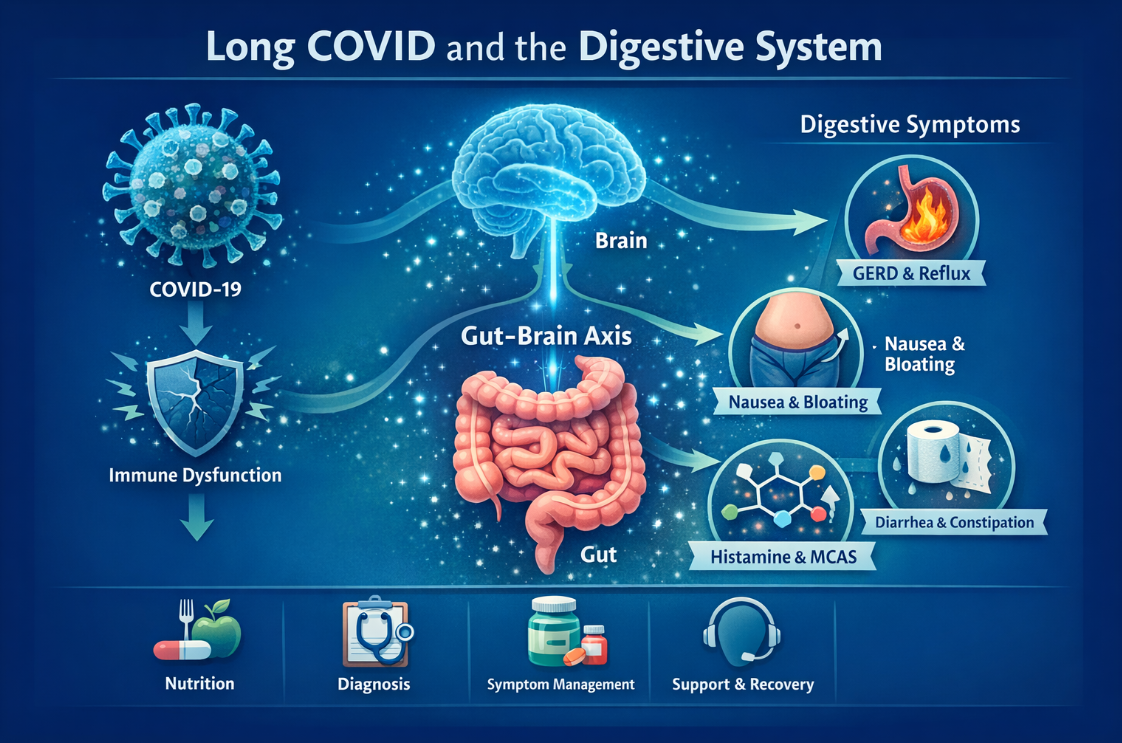
Long COVID and the Digestive System
Many people living with Long COVID report symptoms that affect the digestive tract and gut–brain connection.
These symptoms may appear during the acute infection or develop weeks to months later as part of Post-Acute Sequelae of SARS-CoV-2 Infection (PASC).
Understanding Gastrointestinal Symptoms After COVID-19
The gastrointestinal system contains a complex network of nerves, immune cells, and signaling molecules that interact with the brain and immune system. When COVID-19 disrupts these systems, digestive symptoms can occur alongside neurological, cardiovascular, and immune symptoms.
Researchers increasingly recognize that Long COVID may involve inflammation, nervous system disruption, and immune dysregulation, which can affect the entire digestive system—from the esophagus to the colon.
Why COVID-19 Affects the Digestive System
The SARS-CoV-2 virus enters cells using ACE2 receptors, which are abundant in the gastrointestinal tract. Because these receptors are present throughout the intestines, stomach, and other organs, the virus can directly affect digestive tissues.
In addition to direct infection, Long COVID digestive symptoms may be related to:
• inflammation of the vagus nerve
• disruption of the gut microbiome
• mast cell activation and histamine release
• autonomic nervous system dysfunction
• immune system dysregulation
• serotonin signaling disruption within the gut
The digestive system is closely connected to the nervous system through the gut-brain axis, which means neurological inflammation may also contribute to digestive symptoms.
Common Digestive Symptoms in Long COVID
People experiencing Long COVID frequently report a wide range of gastrointestinal symptoms.
Common symptoms include:
Appetite Changes
Some individuals report loss of appetite, while others experience increased hunger or abnormal cravings. These changes may relate to inflammation affecting metabolic signaling or hormone regulation.
Gastroesophageal Reflux Disease (GERD)
Many Long COVID patients report worsening reflux symptoms, including:
• heartburn
• chest discomfort
• regurgitation
• throat irritation
Inflammation affecting the esophagus or vagus nerve signaling may contribute to these symptoms.
Constipation
Constipation may occur due to slow intestinal motility, dehydration, inflammation, or nervous system disruption.
Some patients report difficulty with bowel movements even when fiber intake is adequate.
Diarrhea
Loose stools or chronic diarrhea can occur when inflammation affects the intestines or alters the balance of gut bacteria.
This may also occur in association with mast cell activation or histamine reactions.
Slow Gut Motility (Gastroparesis)
In some individuals, food moves too slowly through the stomach, a condition called gastroparesis.
Symptoms may include:
• nausea
• bloating
• feeling full quickly
• abdominal discomfort
Autonomic nervous system disruption may contribute to this condition.
Indigestion and Abdominal Pain
Some individuals report persistent indigestion, bloating, or abdominal discomfort even after mild meals.
These symptoms may be related to inflammation, altered gut microbiota, or nerve signaling changes.
Histamine Reactions and Mast Cell Activation
COVID-19 may trigger mast cell activation syndrome (MCAS) in some individuals.
Mast cells release histamine and other inflammatory mediators that can affect the digestive system.
Symptoms may include:
• stomach pain
• nausea
• diarrhea
• food sensitivities
• flushing
Nausea and Vomiting
Some individuals experience persistent nausea or vomiting, sometimes in cycles.
In rare cases, Long COVID patients have reported cyclical vomiting syndrome, which may be related to autonomic nervous system disruption.
Dysynergistic Defecation
Some individuals experience difficulty coordinating the muscles required for bowel movements.
This condition, known as dysynergistic defecation, may occur when nerve signals between the brain and pelvic floor muscles become disrupted.
Eosinophilic Esophagitis
In rare cases, inflammation involving immune cells called eosinophils can affect the esophagus.
Symptoms may include:
• difficulty swallowing
• food impaction
• chest discomfort
Serotonin Cycle Disruption
Approximately 90% of the body's serotonin is produced in the digestive tract.
COVID-19 may disrupt serotonin signaling within the gut, which can affect:
• mood regulation
• digestion
• intestinal motility
• appetite
This may partially explain why digestive symptoms often occur alongside anxiety, depression, or sleep disturbances.
The Brain–Gut Connection in Long COVID
One important reason digestive symptoms are so common in Long COVID is the close relationship between the brain and the gastrointestinal system, often referred to as the brain–gut axis.
The digestive tract contains its own complex nervous system known as the enteric nervous system, sometimes called the body's “second brain.” This system communicates constantly with the brain through the vagus nerve, immune signaling, and hormones. When inflammation or immune dysregulation occurs after a viral infection like COVID-19, this communication network can become disrupted.
Researchers have found that SARS-CoV-2 can trigger widespread inflammation affecting multiple body systems, including the nervous system, immune system, and digestive tract. In Long COVID, persistent immune activation, mast cell activation, and cytokine signaling may interfere with normal gut function. This can lead to symptoms such as:
nausea
reflux and GERD
constipation or diarrhea
abdominal pain
bloating
slow gut motility (gastroparesis)
Another key factor involves serotonin regulation. Approximately 90–95% of the body’s serotonin is produced in the gastrointestinal tract, where it helps regulate digestion, gut motility, and signaling between the gut and brain. Inflammation affecting the gut lining or immune signaling pathways may disrupt serotonin production and metabolism.
This disruption may contribute not only to digestive symptoms, but also to neurological and psychological symptoms frequently seen in Long COVID, including:
fatigue
anxiety
depression
brain fog
sleep disturbances
appetite changes
Because of this complex interaction, Long COVID is increasingly understood as a multi-system condition involving immune dysfunction, neurological signaling changes, and gastrointestinal disruption.
Understanding the brain–gut connection helps explain why treating digestive symptoms often requires addressing inflammation, nervous system regulation, and overall immune health, rather than focusing only on the stomach or intestines alone.
Supporting the Brain–Gut Axis
Strategies that may support recovery of the brain–gut system include:
Anti-inflammatory nutrition
Managing histamine intolerance or MCAS symptoms
Supporting gut microbiome health
Stress reduction and nervous system regulation
Adequate hydration and sleep
Gentle physical activity within tolerance
Because symptoms vary widely between individuals, working with healthcare providers familiar with post-viral illness and Long COVID can help guide appropriate evaluation and management.
Diagnosis of Long COVID Digestive Symptoms
Diagnosing gastrointestinal issues related to Long COVID can be challenging because symptoms often overlap with other conditions.
Evaluation may include:
• blood tests
• stool testing
• imaging studies
• endoscopy or colonoscopy
• motility testing
• autonomic nervous system testing
Healthcare providers may also evaluate for conditions such as:
• mast cell activation syndrome
• dysautonomia
• gastroparesis
• inflammatory bowel conditions
Nutrition Considerations for Long COVID
Nutrition can play an important role in supporting digestive health and reducing inflammation.
Some individuals report improvement when focusing on:
Anti-Inflammatory Foods
• vegetables and fruits
• omega-3 fatty acids
• whole foods
• fermented foods that support gut bacteria
Low Histamine Diets
For individuals experiencing histamine reactions, reducing high-histamine foods may help reduce symptoms.
Common high-histamine foods include:
• aged cheeses
• fermented foods
• alcohol
• processed meats
Hydration
Adequate hydration supports digestion and bowel function.
Plain water is often recommended over sugary beverages.
Smaller, Frequent Meals
Some individuals with slow motility or gastroparesis find it helpful to eat smaller meals more frequently to reduce digestive strain.
Symptom Management Strategies
While research is ongoing, some individuals find symptom relief through supportive strategies such as:
• pacing physical activity to reduce inflammation
• stress management and nervous system regulation
• sleep optimization
• gradual dietary adjustments
• medical management under the guidance of healthcare professionals
Because Long COVID symptoms vary widely, treatment approaches may need to be individualized.
The Gut-Brain Connection
The digestive system and nervous system are closely connected through the vagus nerve and enteric nervous system, sometimes called the body's “second brain.”
Inflammation affecting this system may contribute to both digestive and neurological symptoms.
This connection may explain why many Long COVID patients experience combinations of:
• digestive symptoms
• brain fog
• anxiety
• fatigue
Understanding the gut-brain axis is an important area of ongoing Long COVID research.
What support options exist for Long COVID patients?
Many individuals benefit from structured support navigating care, pacing, and recovery planning.
ProMedView offers:
✔ Chronic Illness Coaching & Advocacy
✔ Long COVID Recovery Coaching
These services focus on helping individuals regain stability, communicate with providers, and plan recovery.
References
Gupta A, et al. Extrapulmonary manifestations of COVID-19. Nature Medicine. 2020.
Cheung KS, et al. Gastrointestinal manifestations of SARS-CoV-2 infection. Gastroenterology. 2020.
Nalbandian A, et al. Post-acute COVID-19 syndrome. Nature Medicine. 2021.
Theoharides TC. Mast cells, inflammation, and COVID-19. Journal of Neuroimmunology. 2021.
World Health Organization. Post COVID-19 condition clinical case definition.
NIH RECOVER Initiative. Long COVID research program.
Carabotti M, Scirocco A, Maselli MA, Severi C., The gut–brain axis: interactions between enteric microbiota, central and enteric nervous systems. Ann Gastroenterol. 2015;28(2):203-209.
Nalbandian A et al. Post-acute COVID-19 syndrome. Nature Medicine. 2021;27:601-615. https://doi.org/10.1038/s41591-021-01283-z
Vargas G et al. Gastrointestinal manifestations of COVID-19 and the potential role of the gut microbiome. Nature Reviews Gastroenterology & Hepatology. 2021.
Gershon MD, Tack J. The serotonin signaling system: from basic understanding to drug development for functional GI disorders. Gastroenterology. 2007.