Myasthenia Gravis and Long COVID
Understanding the Autoimmune and Neuromuscular Connection
covidCAREgroup Education Series
Myasthenia gravis (MG) is a chronic autoimmune neuromuscular disorder that causes weakness in skeletal muscles - the muscles responsible for voluntary movement.
While MG is considered rare, interest in this condition has grown since the COVID-19 pandemic, as viral infections are known triggers for autoimmune disorders.
Let’s review what we know and what we don’t.
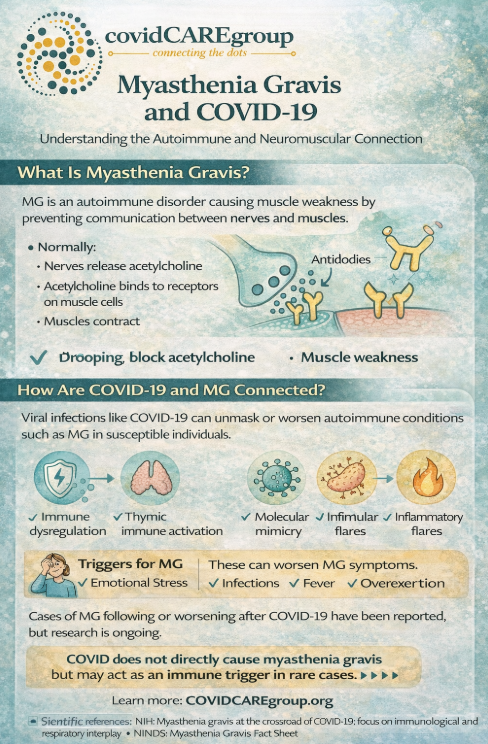
What Is Myasthenia Gravis?
Myasthenia gravis occurs when the immune system produces antibodies that interfere with communication between nerves and muscles.
Normally:
• Nerves release acetylcholine
• Acetylcholine binds to receptors on muscle cells
• Muscles contract
In MG:
• Antibodies block or destroy acetylcholine receptors
• Nerve signals cannot effectively activate muscle fibers
• Muscle weakness results
This weakness typically worsens with activity and improves with rest.
Common Symptoms
MG often begins with:
• Drooping eyelids (ptosis)
• Double vision
• Facial weakness
• Difficulty chewing or swallowing
• Slurred speech
As the condition progresses, it may affect:
• Arms and legs
• Neck muscles
• Respiratory muscles
Weakness tends to fluctuate and worsen throughout the day.
Is COVID-19 Linked to Myasthenia Gravis?
Viral infections are well-recognized triggers for autoimmune diseases — including MG.
Research has identified cases of:
New-onset MG following COVID-19 infection
MG exacerbations in previously diagnosed patients
Respiratory complications due to overlapping muscle weakness and viral lung disease
Proposed mechanisms include:
Immune dysregulation
Molecular mimicry (viral proteins resembling self-proteins)
Cytokine-mediated inflammation
Thymic immune activation
However:
COVID-19 does not directly cause MG in most individuals.
It may act as a trigger in susceptible individuals.
Infections can unmask or trigger autoimmune conditions but they are not the sole cause.
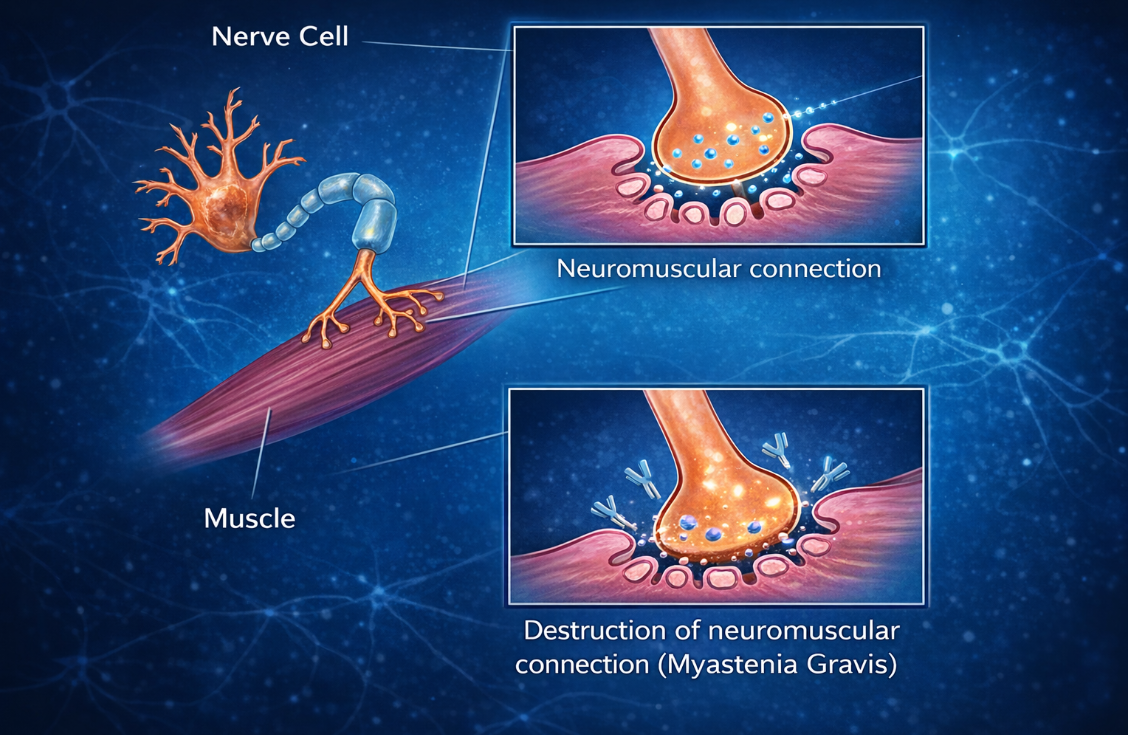
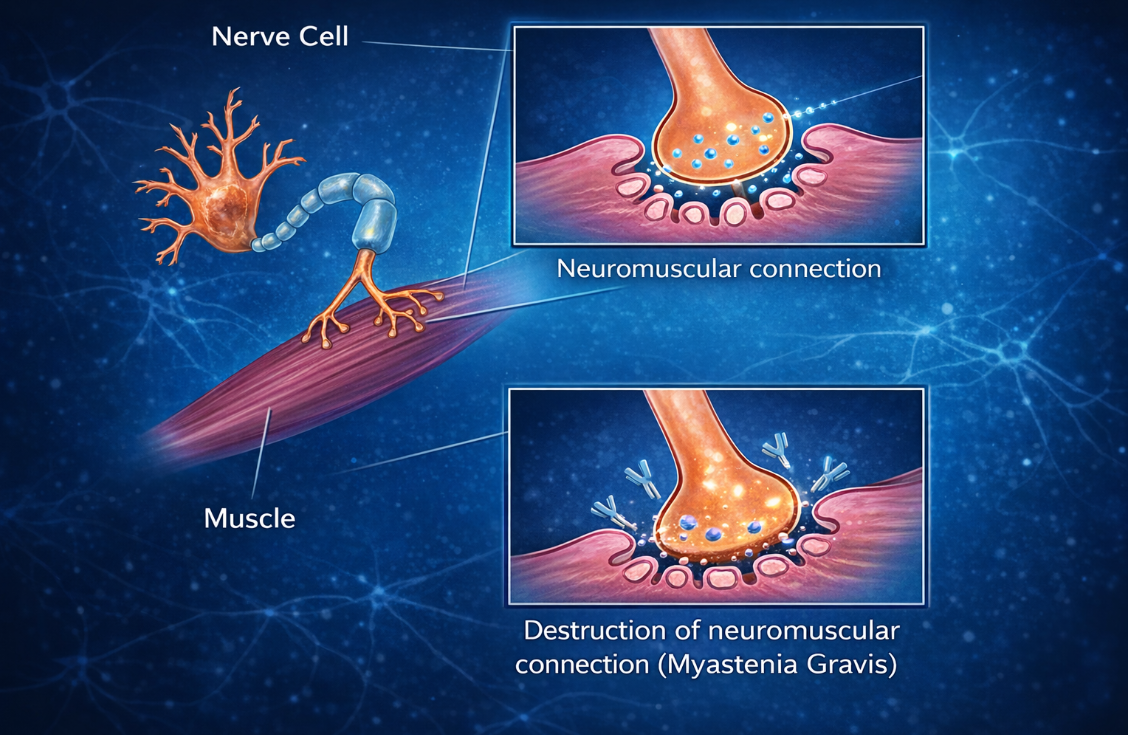
Neuromuscular Junction in Health vs. Myasthenia Gravis
A normal neuromuscular junction (left) vs one affected by myasthenia gravis (right). In a healthy junction, nerves release the neurotransmitter acetylcholine, which binds to receptors on the muscle surface and allows the muscle to contract efficiently. In myasthenia gravis, autoimmune antibodies damage or block these acetylcholine receptors, reducing the signal between the nerve and muscle. As a result, fewer receptors are available to receive the signal, leading to impaired muscle activation and the muscle weakness characteristic of MG.
What About Mast Cell Activation (MCAS)?
COVID-19 is associated with mast cell activation and histamine release in some individuals. While MCAS contributes to inflammation and autonomic symptoms in Long COVID, it is not established as a direct cause of myasthenia gravis.
MG is primarily an antibody-mediated autoimmune disorder targeting neuromuscular junction receptors.
That said:
Inflammation can worsen autoimmune instability
Immune dysregulation can contribute to disease flares
Viral immune activation may increase symptom severity
More research is needed to clarify these relationships.
Risk Factors for MG
MG is rare, affecting approximately 20 per 100,000 people.
It is more commonly diagnosed:
In women under 40
In men over 50
In individuals with thymus gland abnormalities
In those with a family history of autoimmune disease
Diagnosis
Evaluation typically includes:
Neurological exam
Acetylcholine receptor antibody blood test
Repetitive nerve stimulation testing
Pulmonary function tests
Chest CT or MRI (to evaluate thymus gland)
The Edrophonium (Tensilon) test was historically used but is now less common.
Treatment Options
There is currently no cure for MG, but treatments help manage symptoms.
Medications
Cholinesterase inhibitors (Pyridostigmine) – improve nerve-muscle signaling
Corticosteroids (Prednisone, Methylprednisolone)
Immunosuppressants
Biologic therapies in advanced cases
Procedures
Thymectomy
Plasma exchange
Intravenous immunoglobulin (IVIG)
Nutrition & Lifestyle Considerations
Because MG affects chewing and swallowing:
Helpful strategies include:
Moistening solid foods
Choosing soft proteins (fish, poultry)
Avoiding dry, crumbly foods
Eating smaller, more frequent meals
General immune-supportive habits remain important:
Adequate hydration
Sleep hygiene
Stress management
Exercise within tolerance
These do not cure MG — but they support overall resilience.
Potential Complications
Myasthenic Crisis - Life-threatening respiratory muscles weakness. Symptoms: Shortness of breath; Difficulty breathing; Inability to clear airway. Requires emergency care.
Thymoma - Tumor of the thymus gland (associated in some MG cases).
Thyroid Disorders - Both hypothyroidism and hyperthyroidism occur more frequently in MG patients.
Is MG Preventable?
MG is not preventable.
However, known triggers for exacerbations include:
Emotional stress
Infections
Fever
Overexertion
Certain medications (muscle relaxants, some antibiotics)
Extreme temperatures
Managing these triggers can reduce flare risk.
COVID-19 Considerations for MG Patients
Individuals with MG may face increased risk from COVID due to:
Respiratory muscle weakness
Immunosuppressive therapies
Increased vulnerability during infections
Vaccination decisions should be discussed with a neurologist.
What Support Options Exist for Long COVID Patients?
Many individuals benefit from structured support navigating care, pacing, and recovery planning.
ProMedView offers:
✔ Chronic Illness Coaching & Advocacy
✔ Long COVID Recovery Coaching
These services focus on helping individuals regain stability, communicate with providers, and plan recovery.
Final Thoughts
Myasthenia gravis is a rare but serious autoimmune neuromuscular disorder.
COVID-19 may act as an immune trigger in susceptible individuals — but it is not a simple cause-and-effect relationship.
Understanding immune balance, infection risk, and neuromuscular symptoms is key.
As always, covidCAREgroup remains committed to connecting the dots between emerging science and lived experience — responsibly.
Scientific References
NIH: Myasthenia gravis at the crossroad of COVID-19: focus on immunological and respiratory interplay
National Institute of Neurological Disorders and Stroke (NINDS) – Myasthenia Gravis Fact Sheet
Gilhus NE. Myasthenia Gravis. N Engl J Med.
Case reports of new-onset MG following COVID-19 infection